Obesity is defined as excess weight due to an increase in fat mass. It has been recognized as a disease by the WHO since 1997 and is increasingly prevalent in developed countries.
It is defined by a Body Mass Index (BMI) greater than 30 kg/m². Above 40 kg/m², obesity is classified as severe or morbid.
BMI is calculated using the following formula: Weight (kg) / Height (m)²
Severe obesity represents a real health risk, as it may cause:
- Type 2 diabetes
- Sleep apnea
- Arterial hypertension
- Joint or back problems
- Certain types of cancer (colon, breast, uterus, pancreas, …)
The ineffectiveness of so-called conservative treatments (dietary, behavioral, and/or weight-loss programs), as well as the limited long-term effect of anti-obesity medications (GLP-1 inhibitors), have given bariatric surgery an increasingly important role in the management of obesity. Indeed, surgical treatment currently represents the only solution that allows, in the majority of operated patients, for significant weight loss that can be maintained in the long term.
To ensure that the results meet patients’ expectations as closely as possible, it is essential that this surgery be performed within specialized multidisciplinary teams experienced in the comprehensive management of obesity, so that both patient selection and preparation for the surgical procedure are optimized. Dr. Allemann is one of the referring surgeons at the CMCO, the Obesity Medical-Surgical Center, in collaboration with Clinique La Source.
After surgery, follow-up is extremely important. It ensures the limitation of late complications and the maintenance of long-term weight loss. It includes, among other things, monitoring and correction of potential vitamin deficiencies, evaluation of food tolerance, encouragement of physical activity, correction of eating behavior disorders, and dietary counseling.
Types of Procedures
The mechanisms of action of bariatric procedures can be divided into three:
- Restrictive procedures (sleeve gastrectomy, gastric banding)
- Malabsorptive procedures (jejunoileal bypass, biliopancreatic diversion)
- Mixed procedures (gastric bypass). Other hormonal and/or humoral effects are also present but remain poorly understood.
In Switzerland, the two most commonly performed procedures are
GASTRIC BYPASS
This procedure combines an intestinal bypass with the creation of a small gastric pouch of 30 to 50 ml. It is therefore considered a mixed procedure.

Characteristics
It combines restriction with moderate malabsorption. Food absorption is reduced by shortening the functional length of the intestine. Two connections (anastomoses) are required: one between the small gastric pouch and the intestine, and another within the intestine.
How is the procedure performed?
The procedure is performed laparoscopically (5 to 6 small skin incisions are required). The operative time is approximately 1.5 hours. The hospital stay is usually 2 to 3 days.
At Clinique La Source, Dr. Allemann performs this procedure using the Da Vinci robot. This helps reduce operative time, procedure-related costs, and postoperative pain.
Benefits and Advantages
Weight loss is rapid, occurring mainly during the first year. No part of the digestive tract is removed.
Expected Weight Loss
Weight loss amounts to approximately 70–75% of excess body weight. Long-term results have been documented for over 10 years.
Vitamin and Nutritional Deficiencies
Common deficiencies include vitamin B12, vitamin D, and iron, which are easily supplemented. Rare deficiencies involve vitamins B1, B6, and C. Nutritional deficiencies are uncommon.
SLEEVE GASTRECTOMY OR LONGITUDINAL GASTRECTOMY
This procedure involves removing approximately two-thirds of the stomach to create a gastric tube. Food then passes more quickly into the intestine.
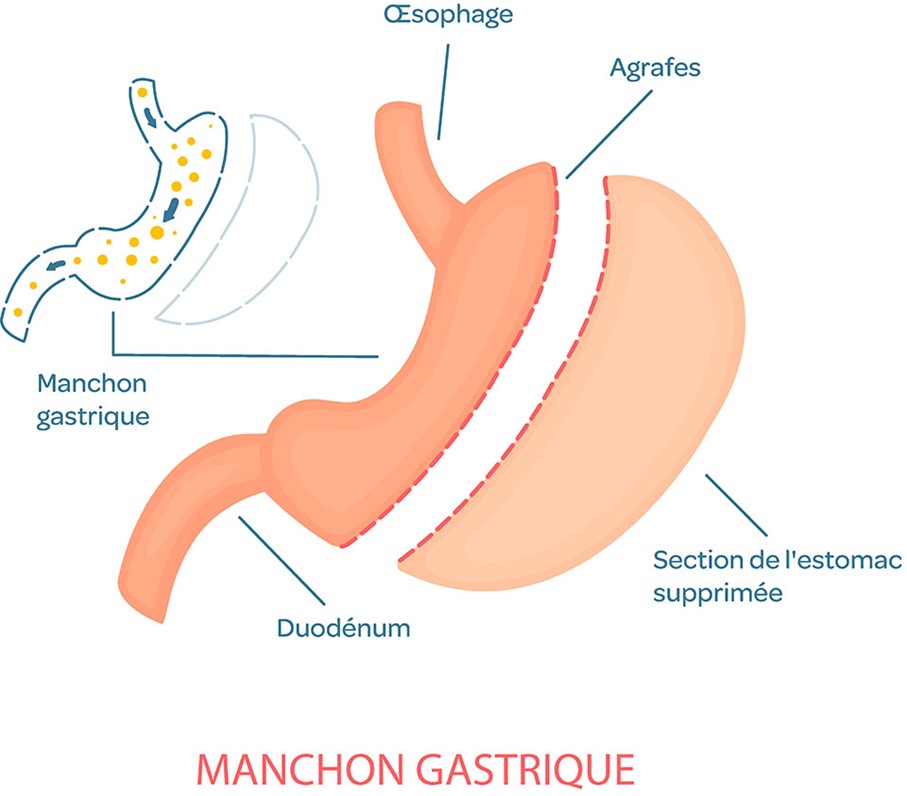
Characteristics
This procedure is restrictive as it reduces gastric volume and induces an early sensation of satiety. It also triggers a hormonal mechanism by decreasing the number of cells that secrete ghrelin, the appetite hormone.
How is the procedure performed?
The procedure is carried out laparoscopically (5 to 6 small skin incisions are required). The operative time is approximately 1 hour.
The hospital stay is usually 2 to 3 days.
At Clinique La Source, Dr. Allemann performs this procedure using the Da Vinci robot. This helps reduce operative time, procedure-related costs, and postoperative pain.
Benefits and Advantages
This is a simple and fast procedure with a low risk of operative complications. The resected portion of the stomach is removed. There is no change in the food pathway. The passage of food into the intestine is accelerated.
Expected Weight Loss
Weight loss is approximately 60–80% of excess body weight. Long-term results have been documented for 10 years.
Vitamin and Nutritional Deficiencies
Possible deficiencies in vitamin B12, vitamin D, and iron. Other nutritional deficiencies are generally not observed.
Complications
Complications may be general and occur in approximately 3% of patients. These may include pulmonary embolism, infections (which may appear early or several weeks later), or hemorrhage.
Complications may also be more specific, directly related to the procedure performed.
A leak at the level of the anastomoses
It presents with abdominal pain, fever, decreased urine output, and tachycardia. Hospital management is then required, and the patient is asked to return to the department where the surgery was performed for diagnosis and treatment. Surgical, radiological, and/or endoscopic intervention may be necessary to manage these complications. Treatment may extend over several weeks.
An infection at the abdominal incision sites
The thickness of the adipose tissue makes healing of abdominal incisions more difficult, and an abscess may develop at these sites. Drainage is performed to allow healing of this localized condition.
A hernia at the surgical incision sites
Despite careful closure of the surgical incisions, rapid weight loss after the procedure weakens the abdominal wall sutures and may result in the development of a hernia. Surgical repair may be necessary and will be provided by our medical team.
Eating disorders, swallowing difficulties
The surgical procedure alters the digestive pathway and requires dietary adaptation. This has been explained during preoperative care and again postoperatively before patient discharge. However, dietary habits can be difficult to change. Most of the time, a clear reminder of the guidelines is sufficient to allow proper nutrition. In rarer cases, a narrowing of the anastomoses between different organs may occur. This may require endoscopic dilation.
Vitamin Disorders
The reduction in food intake and the change in the digestive pathway require regular monitoring of vitamin levels. A multivitamin complex is systematically prescribed upon patient discharge. It should also be noted that vitamin deficiencies may already exist before surgery due to an unbalanced diet. It is therefore essential to follow the consultation schedule with both the surgeon and the endocrinologist to allow for the (easily achievable) correction of these vitamin disorders.
We remain at your disposal for any questions, by clicking on the following link.
Furthermore, we are available for a consultation if you believe that surgery could be a solution to your obesity problem. Dr. Allemann’s practice is one of the entry points to our multidisciplinary network, the CMCO. Please do not hesitate to contact us.