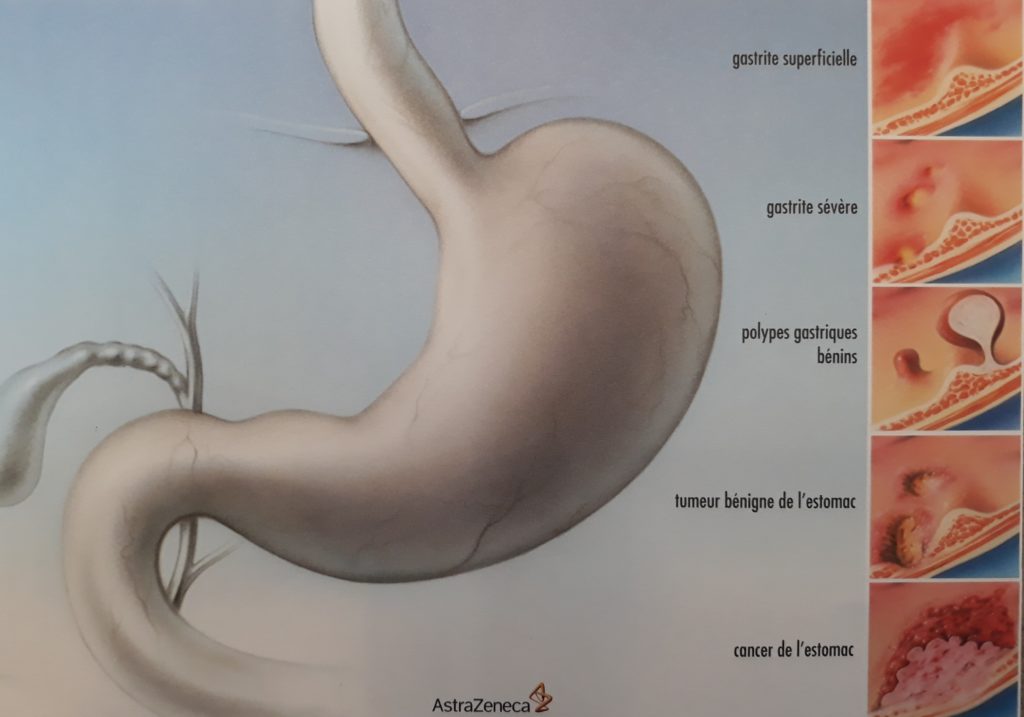
What causes reflux disease?
In most cases, reflux disease results from a dysfunction of the valve located between the esophagus and the stomach: the lower esophageal sphincter. It is classified as a functional sphincter, since it has no specific muscles. Its valve action is ensured by four mechanisms:
– The esophagus enters the stomach at an acute angle (the angle of His).
– The flexible walls of the abdominal portion of the esophagus are compressed by intra-abdominal pressure (like a pinched tube).
– Mucosal folds obstruct the lumen at the gastroesophageal junction.
– The diaphragmatic muscle crura exert a pinching effect.
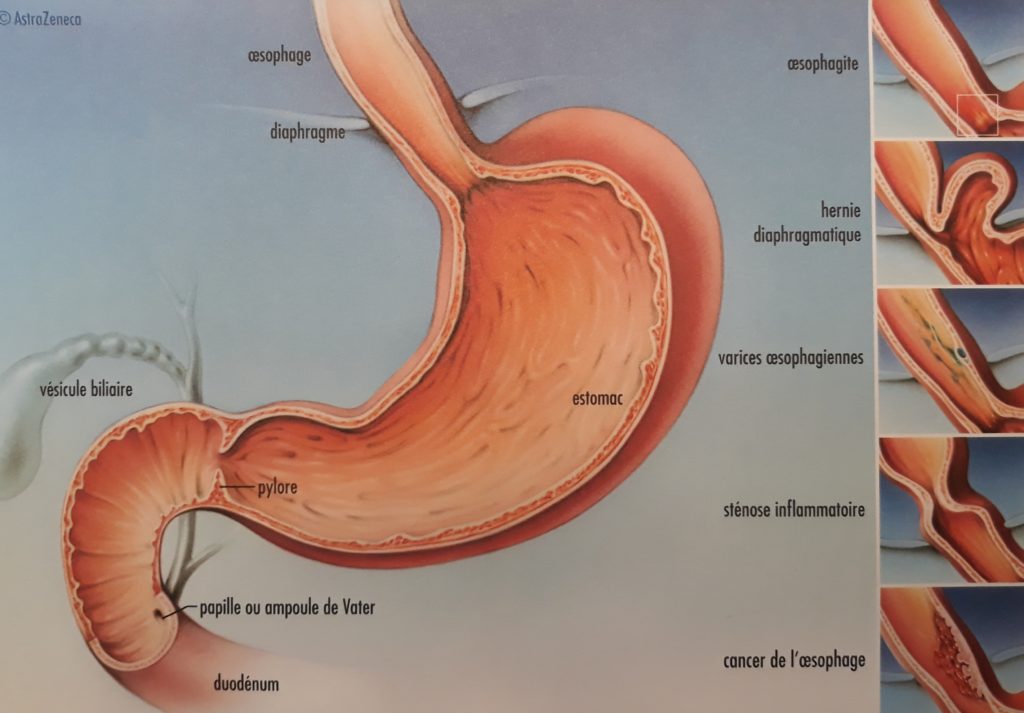
When food is propelled through the esophagus (peristalsis), the sphincter opens to allow it to enter the stomach. Outside mealtimes, this sphincter remains closed, preventing gastric contents from refluxing into the esophagus.
Reflux Disease: What Is It?
Reflux disease occurs when stomach contents flow back into the esophagus (and sometimes even into the mouth). This causes an unpleasant burning sensation known as heartburn (pyrosis). Reflux is very common in the general population.
The most commonly reported symptoms are:
– heartburn or chest burning
– an acidic taste in the mouth
– regurgitation of food into the mouth
These symptoms generally occur after eating, when bending forward, or when lying down.
The Different Types of Reflux
There are two types of reflux: acid and bile reflux. Their origins and treatments are different.
Acid reflux originates in the stomach, one of whose important functions is the secretion of hydrochloric acid. If the sphincter allows gastric contents to pass upward, acid will flow back into the esophagus. This irritation causes the typical pain. Proton pump inhibitors target this type of reflux.
Bile reflux originates in the duodenum, the first part of the intestine after the stomach. In cases of impaired gastric motility, bile may flow back into the stomach. This bile can then also reach the esophagus. Even though its content is not acidic, it remains extremely aggressive to the mucosa.
Very often, both types of reflux can be observed in the same patient. This is referred to as mixed reflux.
How is reflux investigated?
Examinations for assessing reflux can be performed on an outpatient basis. They are conducted and interpreted by a gastroenterologist.
- Gastroscopy (endoscopy, OGD) consists of visualizing the inside of the digestive tract using a camera. It allows biopsies (tissue samples) to be taken for analysis. Through this examination, inflammation of the esophagus or stomach, a hiatal hernia, or cancer can be diagnosed.
- pH-metry measures acidity (pH) in the esophagus. It is the reference test for diagnosing acid reflux.
- pH-impedance monitoring is a variation of standard pH-metry. It measures both types of reflux, acid and bile. This is recorded using a small probe connected to a device, over a period of 48 hours.
- High-resolution esophageal manometry allows visualization of esophageal contractions (peristalsis). This test aims to exclude esophageal motility disorders.
Hiatal Hernia
Normally, the diaphragm (the breathing muscle) separates the thorax from the abdomen. The esophagus passes through it via a small opening, the esophageal hiatus (see Image 1). Sometimes this hiatus is too large (like a hole in the diaphragm), allowing the stomach to move up into the thorax. This is called a hiatal hernia or gastrothorax. There are several types of hiatal hernias (Images 2–5), depending on how much of the stomach, or sometimes other organs, migrate into the thorax.
Type I hiatal hernia is also called a sliding hernia. It is often associated with gastroesophageal reflux disease. The risk of complications is very low.
Type II, III, or IV hiatal hernias are also called rolling hernias or paraesophageal hernias. They are more often associated with symptoms such as chest pain, breathing difficulties, or problems with eating/swallowing. These hernias may present with serious complications such as gastric volvulus, pressure ulcers, and gastric perforation or necrosis.
When Should Hiatal Hernias Be Operated On?
Toutes les hernies hiatales ne nécéssitent pas une intervention. On décidera en fonction du type de hernie et des symptômes.
1) Type I hernia, asymptomatic:
No risk of complications, therefore no surgical indication.
2) Type I hernia, symptomatic:
The surgical indication depends on the associated reflux disease. The hernia itself is not an indication, but it will be corrected during the same procedure.
3) Type II, III, or IV hernia, asymptomatic:
There is no absolute indication, but the benefit of surgery must be weighed against the patient’s risk factors: age, hernia size, and active comorbidities.
4) Type II, III, or IV hernia, symptomatic:
In this situation, surgery is justified, as the risk of developing a serious complication is significant.
What does the operation involve?
At present, there is no standardized technique universally recognized. The only certainty is the superiority of the laparoscopic approach compared to open techniques: fewer complications, shorter hospital stays, and better quality of life. The different surgical steps include:
– Excision of the hernia sac: If present, the peritoneal sac must be separated from the mediastinal structures (particularly the esophagus) and preferably excised completely. Great care must be taken not to injure the vagus nerve.
– Repositioning of the gastroesophageal junction into the abdominal cavity: At the end of the dissection, the gastroesophageal junction, without traction, should be positioned within the abdominal cavity for at least 2–3 cm. For this, the esophagus may need to be mobilized up to the inferior pulmonary veins, if necessary.
– Fundoplication: This procedure involves wrapping the upper part of the stomach around the junction like a tie (thus reconstructing the deficient sphincter). There are two types of valves: partial (Toupet) or complete (Nissen-Demeester). The literature has not demonstrated clear advantages of one type of valve over the other.
In cases of severe esophageal motility disorders, other anti-reflux techniques may be proposed, such as electrical stimulation of the sphincter (EndoStim™), in which Dr. Allemann is a specialist.
| Chaîne YouTube | Articles médicaux | Présentations |
|---|---|---|
Vous trouverez différents films sur la chirurgie digestive minimale invasive. Si vous aimez, n’oubliez pas de vous abonnez à la chaine! | Vous trouverez la liste des publications du Dr Allemann sous la rubrique publications. Article sur la maladie de reflux : lien Article sur la hernie hiatale : lien | Présentations (format pdf) |