General information
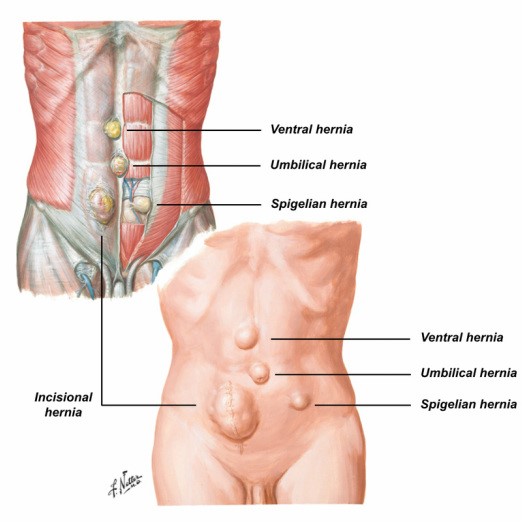
Abdominal hernias are common. A hernia occurs when abdominal contents (intestines or fat) protrude through an opening (hole) in the abdominal wall.
Hernias often present as a lump under the skin, which may increase in size when coughing or straining during bowel movements. They are favored by repeated physical exertion, heavy lifting, obesity, chronic cough, or constipation.
There are several types of hernias, depending on their location:
Inguinal hernia: This is the most common type, accounting for 90% of hernias. It is characterized by a lump, sometimes painful, in the groin fold or scrotum.
Umbilical hernia: Seen in 2 to 10% of patients (more frequently in cases of liver disease such as cirrhosis). It presents as a lump at the umbilicus.
Epigastric hernia: Located above the umbilicus, along the linea alba (in the midline of the abdominal muscles).
Femoral hernia (or crural hernia): The rarest type, about 4% of hernias. It presents as a lump at the junction between the groin and the upper thigh (just below the inguinal hernia).
How to make the diagnosis
The diagnosis is most often clinical. The patient is examined both standing and lying down. Sometimes, coughing provokes pain or an increase in the size of the hernia.
In obese patients, or in the case of a femoral hernia (which is more difficult to diagnose), an ultrasound or a CT scan may be required to confirm the diagnosis.
Treatment
Since this is a mechanical problem (a defect in the abdominal wall), treatment is surgical and consists of repairing the torn tissues, sometimes with the use of a mesh.
Important! Hernias that do not cause symptoms (such as discomfort or pain) are generally not operated on, as they carry a very low risk of complications and are usually managed with observation only.
Surgical intervention is therefore indicated only in women or in men with a symptomatic form.
There are 2 types of techniques:
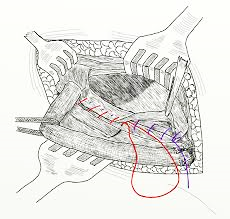
Direct suture: The hernia contents are returned into the abdomen, and the edges of the defect are brought together with a suture.
This is a simple technique, without foreign material, but with a higher recurrence rate (about 10–15% at 5 years).

Reinforcement with a mesh: Here as well, the hernia contents are returned into the abdomen. To strengthen the repair, a synthetic mesh (usually Nylon, an inert and non-absorbable material) is placed.
This technique is considered the surgical standard and helps reduce the risk of recurrence (about 0.5–2% at 5 years).
The procedure can be performed in two ways:
Open surgery: the traditional approach, involving a skin incision. This technique is simpler and faster, but is associated with more postoperative pain and a larger scar, depending on the size of the hernia.
It is still performed in specific situations, when no other technique can be offered.
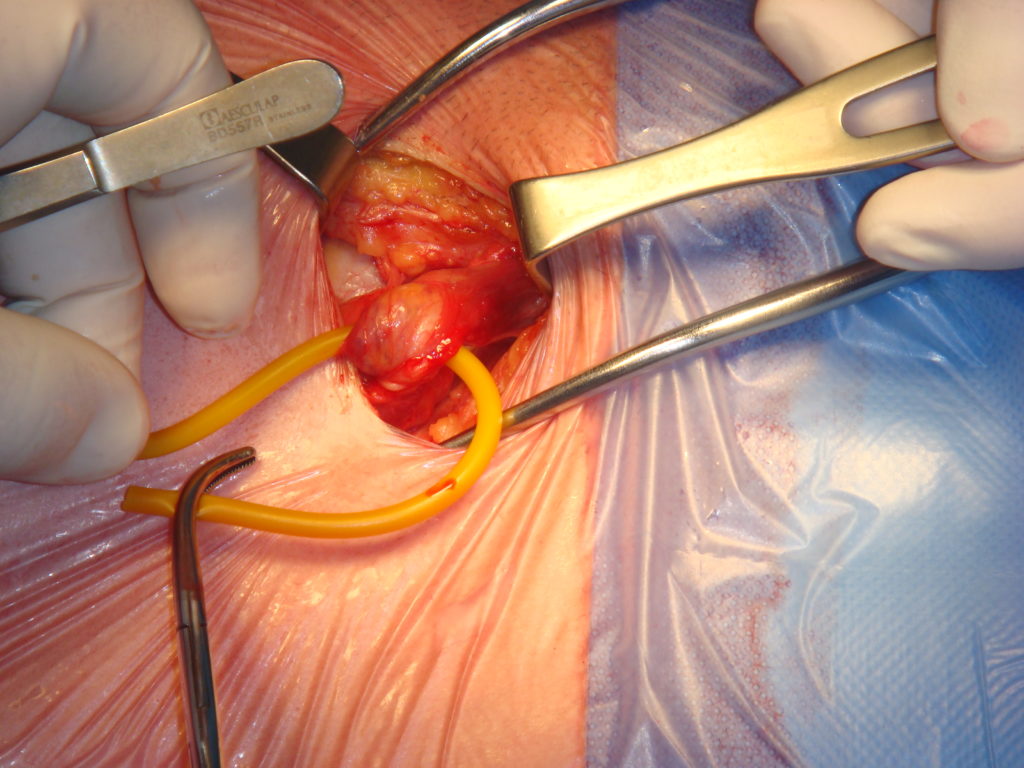
Endoscopic surgery: a minimally invasive technique (also called laparoscopic or coelioscopic). The procedure is performed through small incisions of just a few millimeters. It is technically more demanding, but reduces immediate postoperative pain as well as chronic pain. In addition, return to physical activity (or work) is faster.